
|
|
Simple nail trimming & clearing of the affected corner |
|
|
Examining how your footwear, activity & lifestyle factors may impact the way your nail grows |
|
|
Surgical removal of the ingrown edge under local anesthetic to prevent the corner from growing back. |
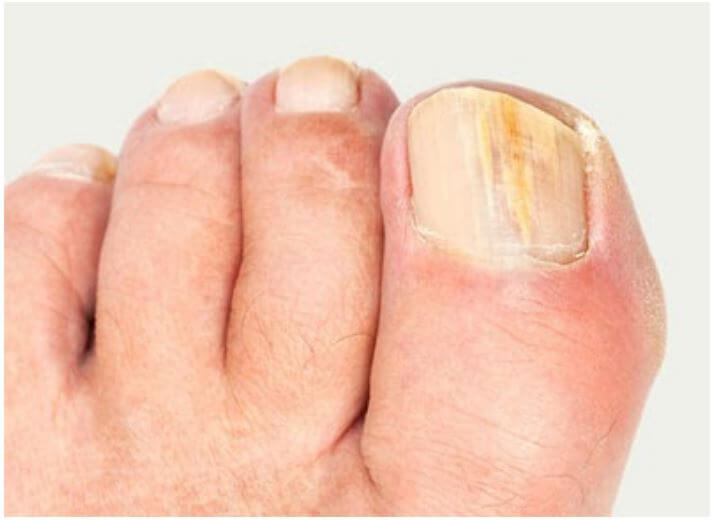
Fungal nail infections are caused when fungi infects the nail plate and the soft tissue beneath the nail. Something as simple as banging a toe, trimming your nails too closely or wearing tight shoes can be enough to weaken the nail and expose the underlying nail bed to infection. Toenails are vulnerable to infection because they can spend much of their day in warm and often moist socks and footwear.
An infection may begin as a white or yellow spot under the tip of your toenail. As the nail fungus spreads, it may cause your nail to discolour, thicken and develop crumbling edges. Thick toenails may cause discomfort in shoes and may even make standing and walking uncomfortable for some people. The infection can spread to other nails, and possibly to other people.
This is best for mild to moderate infections or where oral medicines are preferred or unable to be taken.
A course of treatment is initially 4 treatments, 1 week apart and for more severe infections at least 6 treatments can be needed. It has the highest success rate of all known conservative treatments at around 70%, is painless and with no known side effects.
Click here for more information.
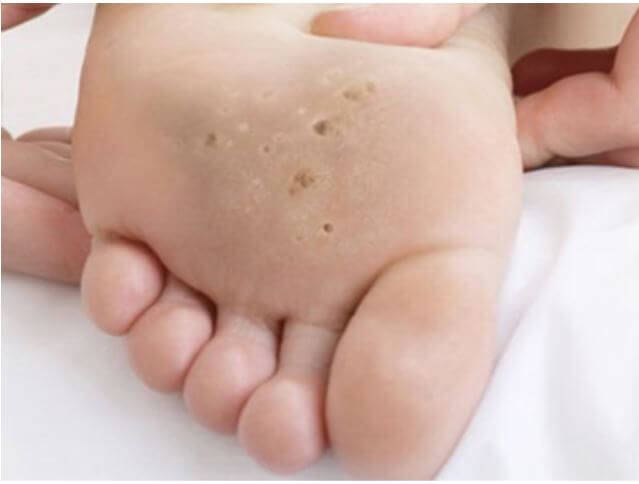
Verrucae are caused by a viral infection and over time, develop into a hard, rough growth on the surface of the skin but can also appear on the top or around the toes. They may appear spongy, with tiny red, brown, or black spots. If left untreated, they can spread to other parts of the foot.
If left untreated, verruca can grow and can form into clusters, these are called mosaic warts. They can be spread by touching, scratching or even by contact with skin shed from another verruca. Verruca may also bleed - another avenue for spreading. Verruca are sometimes mistaken for corns or calluses.
Calluses are hard, thickened areas of skin that are generally not painful and require no treatment. This hardened skin is the body’s way of protecting itself from diffuse pressure or friction. Poorly fitted or worn footwear are a common cause. Some people with dry skin are predisposed to developing callus.
Corns are common foot conditions that occur from repeated focal pressure on the foot, such as rubbing of the skin against a shoe, wearing no socks with shoes, or foot deformities. Women are more likely to develop corns due to wearing high heels and less supportive footwear then men. Corns come in three different forms: hard corns, soft corns, and seed corns. Located on the top or outside of the little toe, hard corns look like a compressed patch of hard skin with a dense core. Soft corns are found between the toes while seed corns develop on the heel or ball of the foot. All corns can be painful.
The pain from a corn can be helped instantly by removing the hard skin that has developed, giving relief straight away and on most occasions will be a painless procedure. They can be cured by removing the force which is causing it via improved footwear choices that reduce pressure on the affected area. Deflective padding and digital corn devices are also indicated for treatment.
Over the counter (OTC) corn pads with medication are available but be wary; the salicylic acid on the corn pad can cause a chemical skin burn and possible infection. These are definitely to be avoided by those with diabetes.
Early stages of fissures on the feet, particularly the heel, involve the splitting of the skin to produce unsightly cracks. If heel cracks remain untreated, the cracks can progress into fissures. Cracks only effect the upper layer of the skin called the epidermis, while fissures begin to crack deeper into the skin, just below the epidermis into the dermis. Dry skin is the reason most people assume they have cracking heels, but increased weight, diabetes, neuropathy, poor circulation and poor nutrition can also cause poor foot health. Symptoms of heel cracks and fissures vary from mild to severe. The most apparent symptom is cracks in the epidermis of the heels. Other symptoms include: Dry, itchy heels, hard skin on the heels, pain, difficulties standing or walking and bleeding or discharge
With proper treatment, heel cracking will not evolve into fissures. Moisturising the feet twice a day will heal the cracks in most cases. If cream is not helping your Podiatrist is able to remove the hard skin and thickness around the cracked region helping to give initial relief and enable the cream to further soften the skin. In more severe cases you may need additional treatments to keep the skin thickness down alongside daily applications of cream. Regular appointments are recommended here
Visit our FAQs page or send us a message.